SCA or SMA? Ataxia or Atrophy?
“What a terrible thing to learn you have in the middle of your life.” That was my neurologist, my new neurologist, speaking.
In 2012 my first neurologist, Dr. M, diagnosed me with late-onset Friedreich’s ataxia, or at least he reported that he felt I have a form of spinocerebellar ataxia (SCA), a disease that has dozens of forms and is genetic in origin. Dr. M’s work led to insurance approval to conduct an expensive genetic test to identify which ataxia I have. (The approval would not have been granted frivolously, so I underwent three MRIs, one EMG test, many blood labs to eliminate Lyme disease and the many other viruses that could be a cause of my symptoms, and started seeing a cardiologist. The fact of my cardiomyopathy led to approval for the DNA test.) But Dr. M moved to a different practice and I met my new doctor, Dr. K, this month.
Dr. K reviewed the first doctor’s extensive notes and looked at me. “You don’t have Friedreich’s ataxia.” (Dr. M was not much for granting eye contact, so this moment of direct conversation surprised me.) Dr. K asked me about my symptoms and when they seemed to begin to appear, some of which I have written about elsewhere. Since 2005 I have been aware, at first dimly, of a mobility disorder developing in me; today, in 2014, I walk with a cane, stiffly, like I am wearing very tight jeans, have little sensation in my lower legs and even have moments of “body confusion” in which I think I am moving my right leg but my left leg moves. I sway when I stand and fall/walk into walls and my sense of where I am in the world contributes moments of comedy to my day.
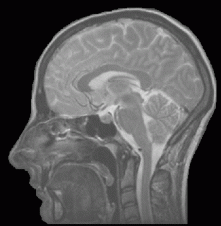
My MRIs show a spinal cord that is shedding its myelin sheath protecting the nerves inside, a couple vertebrae that have spontaneously fused—”When did you have this happen?” Dr. K asked me. “I don’t know,” I replied. “I’ve never had anything done on my back.” “Car accident?” “No.” “Okay, you have a spontaneous fusion”—and places where the nerves themselves are atrophying, withering. But my brain, my cerebellum specifically, it is a healthy brain. I have a fine-looking thinker. Thus, Dr. K posited, I do not have a spinocereballar ataxia, as my cerebellum is healthy.
I spoke in Dr. M’s defense. “I think he was surmising from the tests …” Do not use the words “think” or “surmise” with neurologists. “Ataxia,” Dr. K offered, “has been treated like an umbrella term for patients with movement disorders like yours. But it really is a specific disease and you do not have a spinocerebellar ataxia.” He turned to his computer and started typing what I thought would be yet more patient notes and requests for another battery of tests (Dr. M had generated several pages on my case), but then I noticed what looked like a Wikipedia page on his monitor.
“Based on your labs and the extensive deterioration in your spine and weakness in your legs, you have spinal muscular atrophy, I believe Type IV.” (I swear I heard him say “Type IV” with Roman numerals and in italics.) “Has anyone suggested this to you? No? It may be Type III, but I would say that you have a type called Kugelberg Welander, but very late-onset.” He looked back at me. “You have a genetic disease. What a terrible thing to learn you have in the middle of your life. Your symptoms are severe and I have not seen many adult cases, but you will live, I think, a long life. Your legs will continue to get weaker, but you will adjust.”
(How beautiful is it to have a doctor look in your eye and simply say, “What a terrible thing?” To my first neurologist, a terrific clinician and lab expert, I sometimes felt like I was an interesting case but basically a piece of meat that had the unfortunate habit of speaking.)
“You’re a writer? You’ll probably be teaching me about this by our next visit.”
Spinal muscular atrophy is a genetic disease, a muscular dystrophy that in most cases affects children, but not in my case. The vast majority of spinal muscular atrophy stories are incredibly sad: Type I strikes infants who do not ever control their own movements and eventually suffer respiratory failure and die before age 2. The second type strikes children before age 2 and renders them unable to walk, but most SMA Type II patients live into adulthood. Many children and young adults seen on the annual Muscular Dystrophy Association telethons through the years have had SMA Type II. Type III and Type IV—and there seems to be some debate as to whether there is a Type IV at all—are considered “late onset” and offer patients the lifelong challenge of impaired and deteriorating mobility and, eventually, respiratory difficulty. Since my symptoms struck in my mid-30s and grew aggressive after 40, I seem to be the very picture of an argument for naming a separate Type IV, if what I have is a spinal muscular atrophy.
Dr. K asked about family and friends. I mentioned something about having developed some friendships as a result of reaching out to the online ataxia community (Jason and Kristin: this is me talking about you). “But you don’t have ataxia!” he exclaimed. When he asked if I am still interested in a genetic test to definitively identify what it is I do have, I reminded him that I had been approved for a test for Friedreich’s ataxia. All that test would have shown us, he replied, is that I do not have FA, not what I have.
So one neurologist posited that I have a spinocerebellar ataxia (SCA) of unknown cause and unknown type and another that I have spinal muscular atrophy (SMA), which is rare when it strikes adults but has a relatively gentle prognosis, if a challenging one, with a future of ever decreasing mobility. I know that I do not know. My daily challenges are unchanged by either diagnosis. I could never wish either SCA or SMA on people I detest, but my disease leads me every day to deeper friendships and I hope more patience. Those are both good things. I think I laugh at myself more. I have to.
Since my preliminary diagnosis in 2012, I have been learning about the different ataxias and following the research progress that seems to be unfolding almost every day, especially as it affects Friedreich’s ataxia.
Both FA and the other SCAs and SMA are very serious rare diseases that all too frequently constrain, impair, or even end young lives. But late-onset genetic disease patients, like me, provide a useful, slow-motion version of their disease as it unfolds. As the doctor says in this video here embedded: “The SMA type 3 and type 4 patients are probably going to provide critical information as to the mechanisms of SMA. It is also possible, that a better understanding of the type 3 and type 4 patient, understanding why their disease is so much more benign than the type 1 and type 2 patient, might provide additional windows of insight into therapeutic strategies.”
I have signed up to be listed on the International SMA Patient Registry.